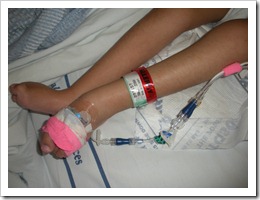
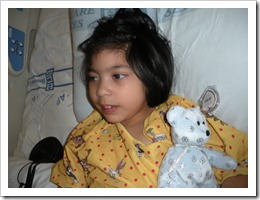
We were finally released from Seattle Children’s hospital on March 13 … 14 days after our admission, 16 days after our first visit to urgent care, 30 days after our first visit to the doctor regarding her “excessive spit up and acid reflux”. It all started from what seemed like a little cold. It reminds us of how the little things affect Jennah so much and how much harder she has to work to do the “normal” things we do, like recover from a cold. These kids are so special and fragile. We learned that a little 2 year old friend, whom we never had the chance to meet, but we anticipated the meeting since we would have back to back therapy times … he very sadly passed away from what seemed like a simple cold. Tragic, scary and so heart-breaking. You hear of people dying of “complications from a cold” … that could have been us.
It’s been 10 days back home and we are finally back into our normal routine, with the exception of returning to school, which we hope to
We’re up to 70 ml/hr on her feeding pump now. She used to be able to breastfeed and take a bottle. 
Of course, we’ve added a couple more medications to her regimen and we’ve had to reassess and recalibrate her seizure meds. We’ll be doing more frequent blood draws to make sure her meds are at a therapeutic level and that her liver is not completely shredded.
I want to say THANK YOU to everybody for their messages of encouragement and prayers. I am especially thankful to those who came to the hospital to visit: mom, Mark, Hubby, A & B, Cassie, Kaye, JennLe, SChai, AArayas, P’Bird, P’Au, Kristi, Kali, Yujin, SK, JamesSu, Trish, Natalie, Thomas, and Holly. I really hope I didn’t miss anyone! And a special thank you to the nurses, doctors, and staff of the Rehab unit … here’s the card we made them:
It all started from a simple cold. As I type, Jennah is sniffling and snorting from yet another cold that she just caught a couple days ago. Colds and little bugs are a lot scarier now. And yes, she has had massive spit-ups (I don’t want to call them vomits just yet).